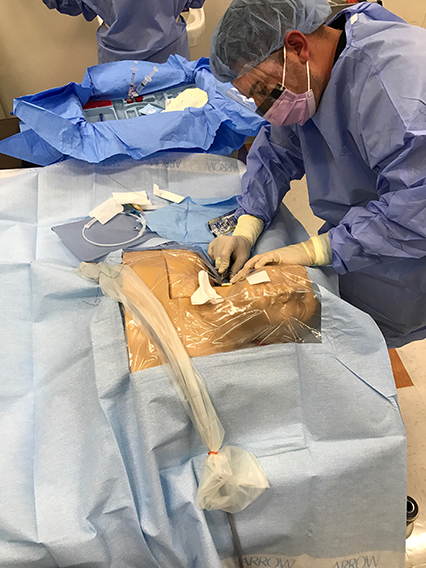
At Midland Health in Midland, TX, RTs have been successfully placing arterial lines since 2010. When the hospital wanted to improve coverage for the placement of central lines in 2016, it just naturally turned to the respiratory care department to take on the job.
This time, however, they are using ultrasound technology to guide the way.
Learning the ropes
JJ Valdez, RRT, RRT-ACCS, who is a member of the ultrasound-guided central line team, says the conversation began in the fall of 2016.
“Not having the resources to provide coverage for central line insertions 24/7, and as a patient safety initiative to reduce hospital-acquired events related to central line acquired bloodstream infections, our facility was seeking a resource that is in-house and available to insert, maintain, and discontinue central lines,” Valdez said.
With support from their department medical director Dr. Gerardo Catalasan and director of cardiopulmonary services Troy Ward, MHST, RRT, Valdez and the other members chosen for the team underwent a five-day course that included 17 hours of didactic training.
Topics included lung ultrasound “knobology,” DVT screening, line insertion, long axis view, orientation to internal jugular placement, chest x-ray interpretation, associated potential complications, femoral vein placement, pneumothorax screening, and line maintenance.
The skills portion of the training increased in difficulty from proper hand placement when using the ultrasound equipment, to the three techniques available for accessing the vessel, to troubleshooting and locating the tip of the needle to redirect it toward the vessel in the event that the needle becomes offline, to the proper process to use once the vessel is accessed.
Refining the skill
The ultrasound-guided central line team began with three RTs and has since expanded to include 10 members.
“Since May of this year we have successfully placed 59 lines, with an 87 percent accuracy rate,” Valdez said. “Initially opportunities were limited, however recently we have seen many more physicians utilize our team and their skillset.”
He says team members who are new to the skill learn from their supervising providers, who offer suggestions and tips for refining the technique.
“Many of us take bits and pieces from each physician to develop a routine that has shown to be most comfortable and most successful for us,” Valdez said.
High expectations
The RTs are most often used for ultrasound-guided central line placement in the critical care areas and Valdez says physician feedback has been increasingly positive, with many expressing their gratitude for the additional resources, particularly during times when their own workload is overwhelming.
Valdez says he is proud to serve on this team, which he believes is helping to advance the profession in a direction that not many saw as a possibility just a few years ago.
While major hospitals with higher designation levels than his facility have anesthesia and surgical residents in-house 24/7 to perform the service, he believes with the right support hospitals like his can benefit from training RTs in the task.
“Our ability to have a team of this nature truly stems from the enormous expectations and highest of standards our medical director and leadership group hold for our division,” Valdez said.





