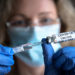
ATS Issues New Statement on Race, Ethnicity in PFTs
The use of race and ethnicity in the interpretation of spirometry results has been called into question by many in the medical community over the past several years. The American Thoracic Society (ATS) has now weighed in with an official statement on the matter based on the findings of a diverse panel of clinicians and investigators convened by the society in 2021 to evaluate the use of race/ethnicity in PFT interpretation, make recommendations, and provide clinical guidance.
Five research articles were subsequently published that provided strong evidence to eliminate the use of race in PFT reporting and interpretation. According to the new ATS statement, race and ethnicity should no longer be considered factors in interpreting PFT results.
The statement has been endorsed by the European Respiratory Society and published online by the American Journal of Respiratory and Critical Care Medicine.
“The recent scientific evidence shows superiority of a race-neutral approach to PFT interpretation for assessing overall and pulmonary prognosis, and for assessing the impact of exposure to tobacco smoke,” said panel co-chair Nirav R. Bhakta, MD, PhD, associate professor, critical care specialist, and pulmonologist at the University of California, San Francisco School of Medicine.
Dr. Bhakta goes on to note that discussion and research in the area is expected to continue. In particular, greater study in more diverse populations is needed to identify modifiable risk factors for reduced lung function and how to measure these factors in a way that could be translated to public policies and pulmonary function testing in the clinic. Read More

Remote Patient Monitoring Reduces Hospitalizations for COPD Patients
Researchers publishing in the International Journal of Chronic Obstructive Pulmonary Disease found that a remote patient monitoring system reduced all-cause hospital admissions by 65% and lowered per-patient all-cause hospitalizations from a mean of 1.09 to .038.
The study involved 126 patients with a mean age of 73.8 who were being treated at a large outpatient pulmonary practice in San Francisco, CA. The remote monitoring system consisted of cardiorespiratory sensors worn under the patient’s clothes that communicated with an in-home data transmission hub. The data transmission hub then sent data to a cloud-based clinical dashboard that could be accessed by the patient’s care team.
Dashboard notifications were issued when the patient’s respiratory rate increased by 10% or the pulse rate increased by 20%, or when 35 breaths per minute or 135 beats per minute were exceeded.
In addition to the 65% drop in all-cause hospitalizations seen in the year after the program went into effect, the investigators noted a 63.6% decrease in hospitalizations due to cardiopulmonary events.
All-cause and cardiopulmonary-related emergency department visits dropped as well, while outpatient care visits rose by 13.2% and prescribed steroids increased by 3.4%. The authors believe the rise in outpatient visits and steroid prescriptions reflected a shift in site of care from hospitals to the outpatient setting that resulted from the use of the remote patient monitoring system.
Adherence to the system was high, with patients wearing the sensors on 88.6% of the days of the study. Read More
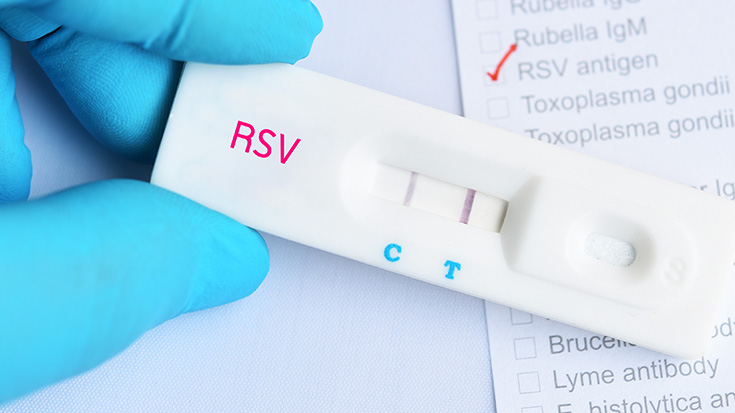
How the Pandemic Impacted RSV
Respiratory therapists, particularly those in children’s hospitals, are well aware of the surge in respiratory syncytial virus (RSV) cases that occurred after the pandemic began to ease up and kids started going back to school and day care centers.
Researchers from Texas A&M University have now put some numbers to the situation in a study published in Frontiers. Overall, the investigators found what while there were an unusually low number of hospitalizations for RSV in 2020, by the third quarter of 2021, hospitalizations for RSV were about twice the number seen in a typical year.
The seasonality of the virus was also affected. While most cases are generally seen in the late fall, winter, and early spring, in 2021 cases spiked in July, August, and September.
Hospital length of stays for RSV were affected by the pandemic too, with longer stays seen during the height of COVID-19 despite fewer cases.
“We can only hypothesize that during COVID they were only accepting the extreme cases, and on average the length of stay was longer,” said study author Itza Mendoza-Sanchez, PhD. “We learned that what has happened in the past is informing us that if something similar happens in the future we have to be ready for the peaks in cases.” Read More
Email newsroom@aarc.org with questions or comments, we’d love to hear from you.